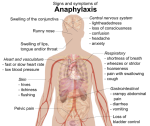
There are a lot of options for treating your allergies but only immunotherapy can keep your symptoms from returning.
Fall is hay fever season so there is a good chance you are experiencing some allergy symptoms. After all, over a quarter of Americans suffer from significant allergies. And for many, the symptoms begin in adulthood. So the question is, what should you do about them? To a large degree, that depends on their severity and your tolerance for discomfort.
Officially, the first course of action is avoidance, which means keeping away from your allergy triggers. In theory that makes sense but it’s often undesirable and all but impossible. For instance, say you’re allergic to the family pet. Are you going to get rid of it even though everyone in the family — including you — loves it? Now consider tree, weed and grass pollen. Even if you move far away from the source of the pollen that’s bothering you, a good stiff breeze will send it flying right to you — tree pollens travel hundreds of miles.
When symptoms start, a majority of people turn to the next courses of action: over-the-counter medications and natural remedies, including nasal irrigation products. Sometimes these measures work very well at relieving symptoms short term. The key here is “short term.” What these products do is overcome your current reaction to allergens. That’s great if you get occasional and/or mild symptoms. There are two “howevers,” though.
The first is the side effect “price tag.” Medications often cause side effects, like drowsiness, that can significant reduce your productivity. And they may not work right away, if at all; doctors now recommend you start taking medications weeks before your symptoms normally start for maximum effectiveness. Even if you do that, the only potential benefit is symptom relief. So you are supposed to take meds in anticipation of symptoms you don’t have yet just to get temporary relief from this year’s onslaught.
The second “however” is even bigger. Let’s say, best case scenario, the medication or natural remedy overcomes your symptoms today. Excellent. But tomorrow when you encounter your allergy trigger — be it pollen, pet dander, mold, etc. — the symptoms start up all over again. You’ll be taking the medication, or using the remedy, for the rest of your life. That’s a lifelong commitment to meds.
There is another option: immunotherapy. This natural treatment exposes your immune system to small amounts of the pollen — or other allergens that your body thinks are enemies — until your immune system learns to accept those allergens as normal. When the body stops trying to fight them off, your allergy symptoms decline and often disappear. In other words, immunotherapy actually makes you better. Every day on immunotherapy is a step towards an allergy-free life.
Immunotherapy doesn’t work overnight. It typically takes a few weeks to two months for treatment to start working. For best long term results, you should continue treatment for three to five years. There are three types of immunotherapy: allergy drops, allergy shots and tablets.
Allergy drops have been popular throughout the world for over 60 years. In the comfort of your home, you simply place a few drops of serum (which is composed of the allergens that trigger your symptoms) under your tongue every day. The drops are convenient, easy, safe, nearly side-effect-free and suitable for allergy sufferers of all ages. The best drops formulations are ones that are designed specifically for you. You start with a low dose and ramp up to a higher dose when your body is ready.
Allergy Shots have been used successfully in the U.S. for decades. Healthcare providers administer the shots to you in their offices on a regular basis, often weekly or bi-weekly. Health insurance policies usually cover many of the out-of-pocket costs associated with allergy shots. Both shots and drops can be formulated to address multiple allergies at once. So, for instance, if you’re allergic to cat dander and tree pollen, you can be treated for both at the same time. Like drops, shots start at a low dose and ramp up.
Tablets are a new form of immunotherapy. Each one is made to combat a single allergen. Unfortunately, most people are allergic to more than one thing. But the companies that makes these tablets have targeted the most severe allergens, like ragweed and grass pollen. Tablets start at full dose, so you get a large amount of allergen under your tongue from day one, ready or not.
So which sounds right for you? If you’re symptoms are mild and very sporadic, and over the counter medications do a good job of hiding them for you without too many side effects, you may choose to go that route. But if they’re more severe, you’re tired of the recurring battle with symptoms, you have side effects with the drugs, or you just don’t want to take medication for the rest of your life, immunotherapy might be your best bet. Either way, you should ask your doctor for an allergy evaluation. You should always be armed with information and a definite diagnosis of allergies before taking even the stuff you can buy over the counter. Once you have answers about the cause, you and your doctor can discuss the right treatment.
.![]()